A six-year-old boy with a potentially life threatening medical issue was sent home untreated after an audio-visual consultation at a Multipurpose Service.
Subscribe now for unlimited access.
or signup to continue reading
Aletha Jones' young son Eli began to complain about feeling unwell from flu-like symptoms one Friday.
She began the usual routine of ibuprofen and paracetamol treatment to help stem his discomfort. As the week progressed his condition worsened.
By the following Friday, he began to suffer from crippling stomach pains.
Mrs Jones made the decision to take him to the emergency department at the Blayney Multipurpose Service to have him assessed.
"He had been vomiting and when they looked at him there they said that he must have caught a tummy bug on top of what he already had," she said.
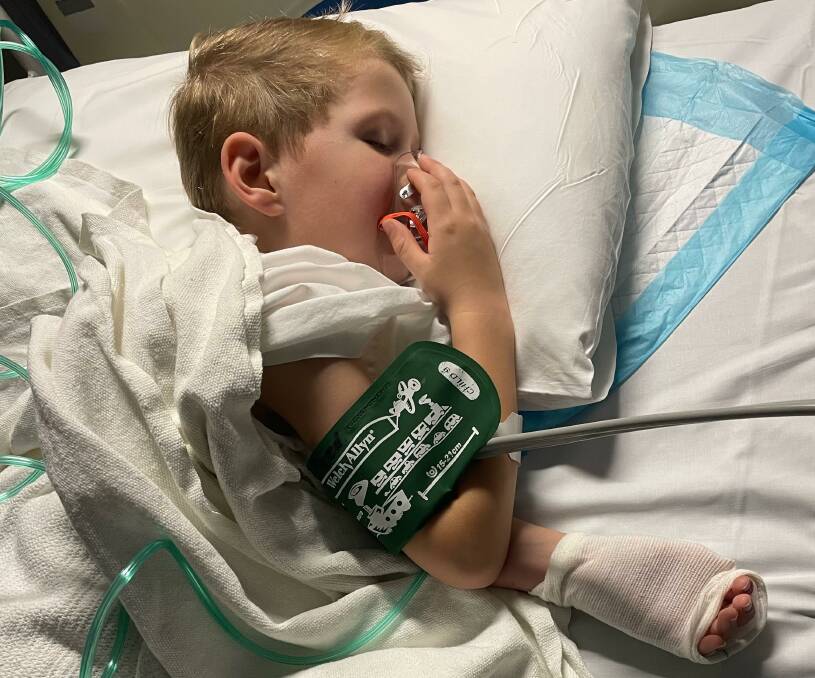
"They gave him some ondansetron to stop the vomiting and told us to give him 20 millilitres of water every hour, but it didn't work."
That consultation was conducted using the MPS audio-visual link with a doctor at Orange Health Service.
The next day Eli still showed no improvement so Mrs Jones asked her husband to take the boy to Bathurst hospital, where it was quickly discovered his condition was much more serious than just a tummy bug.
"He was so badly dehydrated that his ketones were around four or five," she said.
"They then gave him an ultrasound and discovered that he had a ruptured appendix."
If appendicitis is not treated, the appendix can burst and cause potentially life-threatening infections.
Luckily for Eli, 30 minutes after the ultrasound he was in the operating theatre where they discovered the area around the abdomen was full of pus and his abdomen was flushed out.
IN OTHER NEWS:

Mrs Jones said that the staff at Blayney MPS were not even instructed to take any bloods for the consulting doctor to refer to during the AV examination.
"The nursing staff there were wonderful but they needed to do the basics when we were there to check his hydration and sugar levels."
A spokesperson for Western NSW Local Health District said that there has been a long-standing arrangement at Blayney that local doctors are supported by virtual services, including the Virtual Rural Generalist Service.
"Our nursing and bedside teams are extensively trained, highly-skilled and provide exceptional care. Where doctors are not available, they are supported 24/7 by the VRGS, which provides access to experienced, Australian-trained clinicians across a range of disciplines," the spokesperson said.
"Virtual care is in place to support staff, not to replace local doctors, and specialists work with the bedside team to support diagnosis, treatment, admission and, where required, transfer to another hospital.
"Attracting and retaining the required staff, especially GPs willing to provide services in hospitals as VMOs, to regional and rural areas remains a long-standing challenge across Australia."
Reading this on mobile web? Download our news app. It's faster, easier to read and we'll send you alerts for breaking news as it happens. Download in the Apple Store or Google Play.


